According to the Centers for Disease Control and Prevention, 30 million Americans are diabetic, and some don’t even know it. This is a staggering figure, highlighting the grave crises facing the country. Patients that don’t know they’re diabetic can’t follow diabetes management guidelines for their condition. November is National Diabetes Month, which means it’s the perfect time to learn more about this condition.
Diabetes is a chronic disease that causes blood sugar levels to increase due to the body failing to produce enough insulin (a hormone responsible for transporting sugar from your blood into your cells for storage or energy). Another problem related to diabetes is not being able to use the insulin the body makes effectively.
Learning about the disease and following diabetes management guidelines is crucial to controlling blood sugar levels and avoiding other health conditions like damage to tissues, kidneys, eyes, and nerves.
Types of Diabetes
Type 1
Type 1 diabetes occurs when your body’s immune system erroneously starts attacking and destroying cell-producing cells in the pancreas.
Children and teenagers are most likely to be diagnosed with type 1 diabetes, however, if you have a sibling or parent who has it, or you carry genes associated with the condition, you are at risk. Since your body is unable to make insulin, treatment involves taking insulin.
Type 2
This is the most common type of diabetes and results from your body becoming resistant to insulin, thereby causing sugar to accumulate in the blood. Risk factors include:
- Being 45 and older
- Being overweight
- Not being physically active
- Having other conditions like high cholesterol, high blood pressure, or high triglycerides.
Additionally, you’re at a higher risk if you’ve previously had gestational diabetes or prediabetes and if your parent or sibling has the condition.
Prediabetes
Having prediabetes means your blood sugar levels are higher than normal, but lower than what constitutes a type 2 diagnosis. People with prediabetes are at risk of becoming diabetic within 10 years.
Gestational Diabetes
Gestational diabetes occurs when a pregnant woman has high blood sugar. Even if you’ve never had diabetes, you can develop it once you become pregnant.
If you’re older than 25, overweight, have had gestational diabetes before, have polycystic ovary syndrome and have a family history of type 2 diabetes, this increases your risks. After delivering your baby, the condition should go away, however, your risk of getting diabetes in the future becomes considerably higher.
Causes of Diabetes
The causes of diabetes are dependent on the type. Ultimately though, diabetes is triggered by your genes and lifestyle choices.
Type 1 Diabetes Causes
Although the cause of type 1 diabetes is unknown, genes may be the culprit in some cases, or it could also be due to a virus. Type 1 diabetes is caused by factors that cannot be controlled and therefore is not preventable.
Type 2 Diabetes Causes
Genes and lifestyle lead to type 2 diabetes. Family history is a major factor, as genes that make one predisposed to the condition are passed down from generation to generation.
However, your lifestyle also plays a role. Being overweight or obese is a high-risk factor. Extra weight in your belly can make your cells more resistant to the effects that insulin has on your blood sugar.
Causes of Gestational Diabetes
Hormonal changes that occur during pregnancy cause gestational diabetes. Also, being overweight when you fall pregnant or gaining an excessive amount of weight during your pregnancy will increase your chances of getting the condition.
Symptoms
If you are diabetic, the general symptoms you will start to notice include:
- sores that don’t heal
- increased hunger
- increased thirst
- Extreme fatigue
- Blurry vision
- Weight loss that’s unintentional
- Frequent urination
Besides these general symptoms, some symptoms are exclusive to either men and women.
Women may notice their skin becoming dry and itchy, and they may develop a yeast infection or a urinary tract infection. Unfortunately women with gestational diabetes rarely show any symptoms. They often only learn that they have the condition after undergoing a routine blood sugar tolerance test done between 24 and 28 weeks of pregnancy.
Because diabetes symptoms tend to be quite vague, it can be difficult to recognize them initially. However, if you do pick up on any of these symptoms, visit your doctor immediately. The earlier you get diagnosed, the sooner you can start taking measures to control the condition
Diabetes Management Guidelines
Diabetes Diet
You can’t manage diabetes without changing how you eat. Start by creating a meal plan that will help you manage your blood sugar, pressure, and cholesterol. Choose water over sweetened drinks and ensure that you eat smaller proportions. Swap foods high in calories, salt, sugar, trans fat and saturated fat for fruits, vegetables, chicken, fish, olive oil, whole grains, and nuts. A dietician can help you with this.
Get Active
Being active for at least 30 minutes a day a few times a week can make a huge difference. Whether it’s walking, swimming, or cycling, you need to get moving! Exercise is vital because every inch you lose improves your health and prevents your risk of becoming diabetic if you’re not already.
Quit Smoking
The combination of smoking and diabetes narrows your blood vessels, forcing your heart to work harder. Giving up smoking will lower your cholesterol and blood pressure levels, improve your blood circulation and decrease your risk of heart attack, stroke, kidney disease, nerve disease, and diabetic eye disease.
Don’t Forget Your Medicine
Taking your medication for diabetes and other health problems you have is important for the healthy management of diabetes.
Speak to your doctor about what vaccines you need to get (for example flu shots or pneumonia shots) to avoid getting sick, as this can cause your blood sugar levels to go up. Also remember to speak to your doctor about adjusting your medicine’s dosage to complement your fitness routine to prevent excessively low blood sugar.
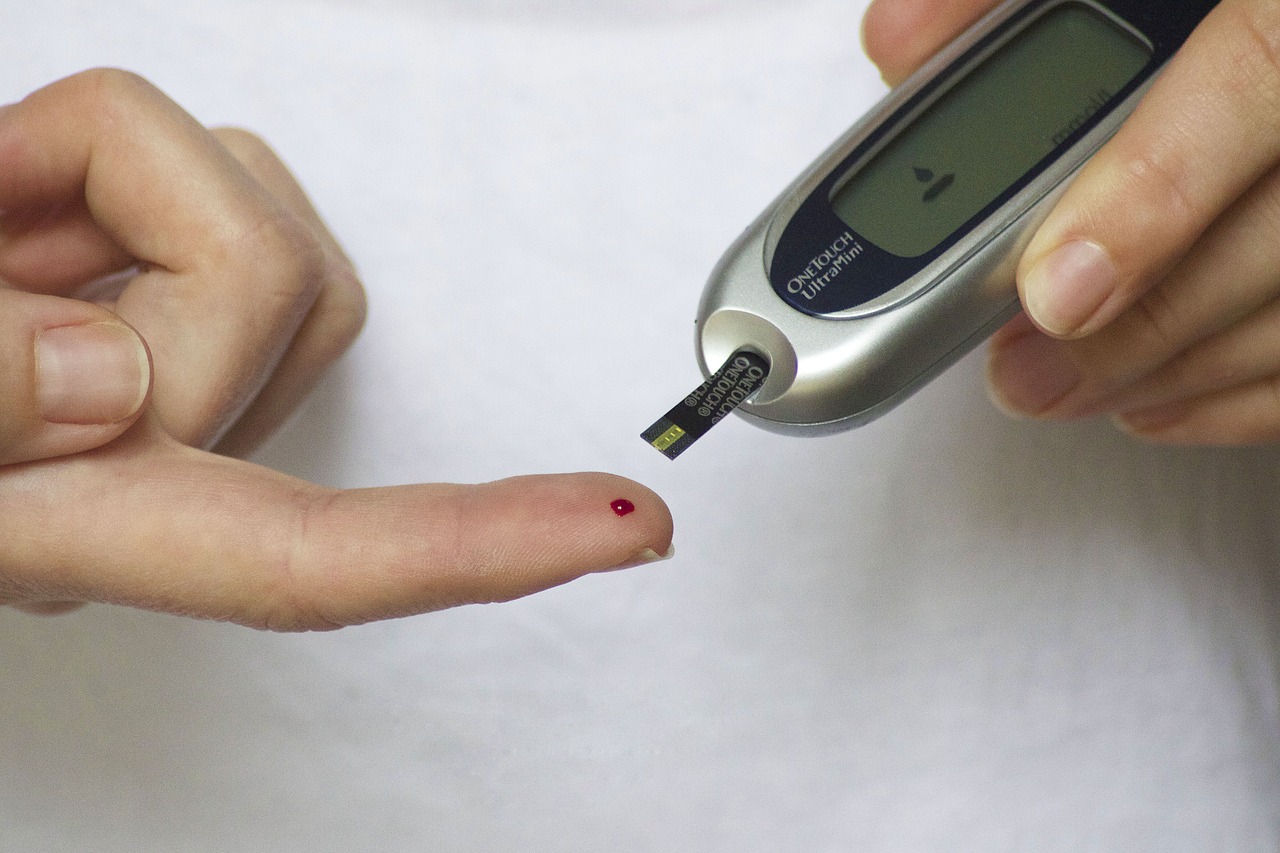
Check Your Sugar Levels
Monitor your blood sugar levels regularly, especially if you’re taking insulin. Keeping track of your sugar levels will assist you in making better choices about your diet, fitness routine, or medication. It will also alert you of when you need to make some changes.
You can use a tool known as a blood glucose meter to check your sugar levels at home. You should aim to stay in the range of less than 100 mg/dL after not eating for 8 hours and less than 140 mg/dL 2 hours after you’ve eaten. Levels above 215 mg/dL are considered high, with the upper acceptable limit being approximately 180 mg/dL.
There’s also another scale for measuring blood sugar levels called the hemoglobin A1C test score. In this scale, measurements between 4-6 are good, 7-8 is acceptable and 9-14 is high.
It’s important that you keep a record of your blood sugar levels. Next time you visit your doctor or health care team, this information will should be readily available.
Mental Health Matters
It’s common to feel sad, stressed, angry, and even depressed when living with diabetes. Nonetheless, stress can increase your blood sugar levels and depression makes disease management more difficult.
Speak to someone – professional or otherwise – who will listen to you and help you to feel better. You can also try doing yoga, starting a hobby, taking walks, meditating, and listening to music to help lower your stress. Getting enough sleep will also help improve your mood.
Home Health Care for Diabetic Patients
Home health aides provide a range of health care services in the home, based on what a patient’s needs are.
For diabetic patients, health aides can assist with:
- Making sure you take your medication on time
- Helping with exercises
- Making sure your weight stays at a healthy mark
- Helping you take care of any slow-healing wounds
- Checking your blood pressure
Health aides can help patients lower the stress that comes with living with a chronic illness, which is also beneficial to the patient.
Consequences of Not Following Diabetes Management Guidelines
Diabetes can bring about new health problems, especially if not managed properly. If your blood sugar levels are very high and remain that way for a long time, this can make you vulnerable to other medical complications, some of which are very serious. Examples include:
- Heart disease and heart attack
- Kidney disease
- Nerve disease
- Dementia
- Foot sores
- Hearing loss
- Vision loss
- Bacterial infections
- Fungal infections
- Stroke
- Depression
Gestational Diabetes Complications
If you have gestational diabetes, your baby can be at risk of premature birth, being born weighing an abnormal weight. Other complications infants from diabetic mothers can suffer from include jaundice, low blood sugar, breathing problems, higher risk of having type 2 diabetes when they get older, and even stillbirth.
Mothers can also develop high blood pressure or type 2 diabetes at a later stage. The possibility of having gestational diabetes in future pregnancies also increases after one occurrence.
In Conclusion
Diabetes may be a complicated disease, but it’s manageable. All it takes is putting a little effort into your health every day. Whether you’re diabetic or not, take the time to learn about diabetes management guidelines so that you can stay ahead of the disease. And remember, it is possible to continue living a healthy life with diabetes.